 In the United States, the most frequently identified risk factors for HAV infection vary from year to year. Determining HAV endemicity globally is complex, however, and limited data are available on subpopulation variation of HAV antibody seroprevalence within regions ( Map 5-06). In areas of low endemicity (e.g., western Europe, the United States), infection is less common, but disease occurs among people in high-risk groups and as communitywide outbreaks. In areas of intermediate endemicity (e.g., Central and South America, eastern Europe, parts of Asia), childhood transmission is less frequent, more adolescents and adults are susceptible to infection, and outbreaks are more likely. In highly endemic areas (e.g., parts of Africa and Asia), a large proportion of adults in the population are infected as children, are immune to HAV, and epidemics are uncommon. Hepatitis A is common in areas with inadequate sanitation and limited access to clean water. 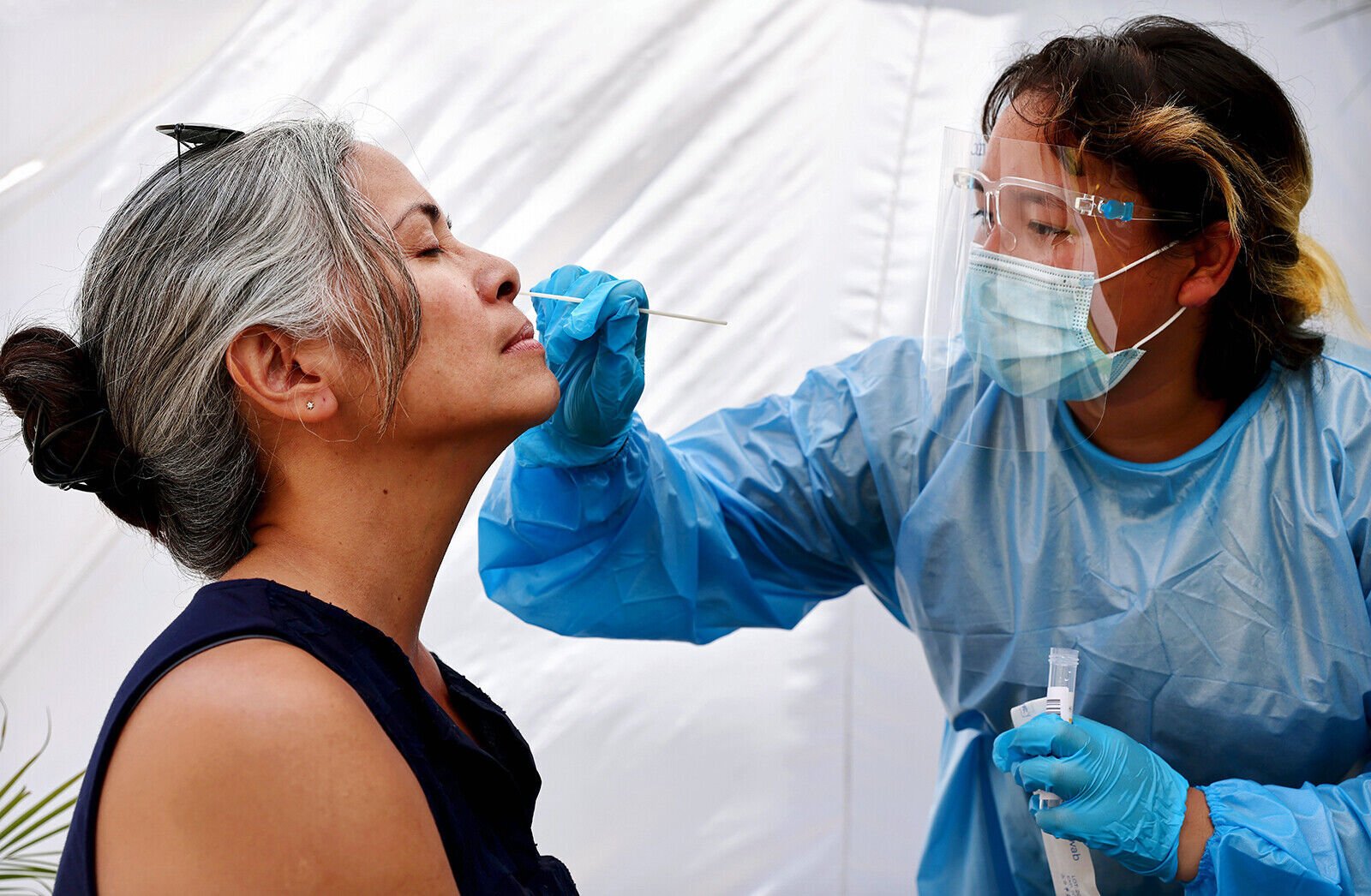
Multinational hepatitis A outbreaks among men who have sex with men (MSM) have been described, including, since 2016, among MSM who travel to areas in European Union countries with ongoing HAV transmission among MSM. Common-source food exposures are increasingly recognized as a risk for hepatitis A, and sporadic outbreaks have been reported in Australia, Europe, North America, and other regions with low levels of endemic transmission. Risk is greatest for those who live in or visit rural areas, trek in backcountry areas, or frequently eat or drink in settings with poor sanitation. 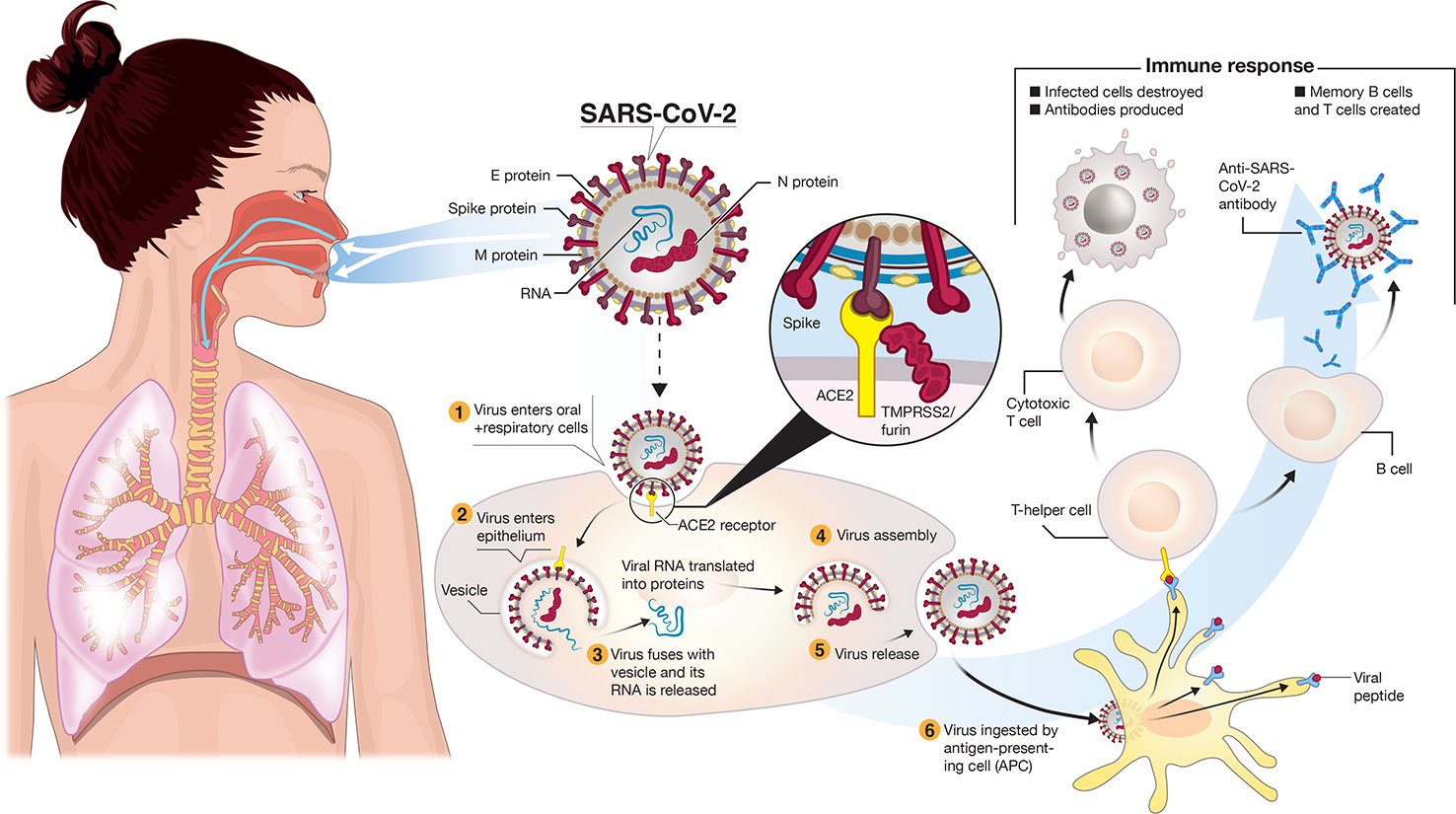
Cases of travel-related hepatitis A can occur in travelers to developed and developing countries and who have standard tourist accommodations, eating behaviors, and itineraries. Hepatitis A is among the most common vaccine-preventable infections acquired during travel. Infants and children can shed virus for up to 6 months after infection. 
Viral excretion and the risk for transmission diminish rapidly after liver dysfunction or symptoms appear, which is concurrent with the appearance of circulating antibodies to HAV. People are most infectious 1–2 weeks before the onset of clinical signs and symptoms of jaundice or elevation of liver enzymes, when virus concentration is greatest in the stool and blood. Recent large-scale outbreaks have been caused by common-source food exposures (e.g., frozen berries, fresh fruit and vegetables, seafood) and through person-to-person spread among people experiencing homelessness and people who use injection and non-injection drugs. HAV can be transmitted from raw or inadequately cooked foods contaminated during growing, processing, or distribution, and through contamination by an infected food handler. Heat inactivation must occur at temperatures >185☏ (>85☌) for 1 minute. Freezing does not inactivate the virus, and HAV can be transmitted through ice and frozen foods. HAV can survive in the environment for prolonged periods at low pH. 
HAV is transmitted through direct person-to-person contact (fecal–oral transmission) or through ingestion of contaminated food or water. Hepatitis A virus (HAV) is a nonenveloped RNA virus classified as a picornavirus. For more information, please visit CDC's Test Directory webpage. A clinical laboratory certified in moderate complexity testing state health department or for testing at CDC. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
